COVID-19 Guidance for Residents, Residency Directors/Mentors, and Administrators
Thanks to the support of the O&P school faculty, we are pleased to announce that O&P graduate preparedness information is available for graduates from all CAAHEP accredited programs. PDF copies with reports from your current residents’ alma mater are sent via email to the residency program directors during the first week of each month (with the initial batch being sent in July). The next set will be sent out during the first week of August. If you are a residency director and would like to request an additional copy for a current resident whose academic training was affected by COVID-19, please contact the NCOPE residency staff at residency@ncope.org.
Purpose of This Document: This information is designed to provide guidance and resources for all NCOPE accredited residency program stakeholders including future/current residents, clinical faculty, and practice administrators regarding residency training during the continued spread of the novel coronavirus (COVID-19). Although it is not possible to account for all unique circumstances faced by O&P clinical facilities nor the future, NCOPE would like to provide clear information to help direct the ongoing training of future orthotists/prosthetists. We will continue to monitor guidance from the Department of Education (DOE), Center for Disease Control (CDC) , and World Health Organization (WHO) about the Novel Coronavirus (COVID-19) and will update this page to keep stakeholders informed during these challenging times.
Be Prepared
Be aware of the local COVID-19 environment. Seek input from local, state, and federal authorities to ensure your clinical practice is operating legally and in a manner that protects the interest of the patients, staff, and the public.
-
- Directory of Local Health Departments: https://www.naccho.org/membership/lhd-directory
- CDC COVID-19 Information Page: https://www.cdc.gov/coronavirus/2019-ncov/index.html
Review and refine your organization’s infectious disease control and safety plan. Take steps to ensure your infectious disease control and safety plan accounts for the current COVID-19 outbreak. Protect the well-being of your staff while providing essential care to persons potentially infected with the virus.
-
- ABC Coronavirus Information Page: https://www.abcop.org/news-events/CurrentNewsandEvents/2020Archive/Pages/Message-from-ABC-Regarding-Coronavirus.aspx
- BOC Coronavirus Information Page: https://www.bocusa.org/covid-19
- CDC Guidance of Preventing Spread of Coronavirus/PPE: https://www.cdc.gov/coronavirus/2019-ncov/infection-control/control-recommendations.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcoronavirus%2F2019-ncov%2Fhcp%2Finfection-control.html
- ISPO Suggestions for Providing O&P Care During the COVID-19 Pandemic: https://drive.google.com/file/d/1FPizfu-pB6nDEBKueBgEtBI-6-nry5eu/view
Triage and screen patients to ensure access to essential O&P care. Follow guidance from affiliated hospitals, clinics, and agencies to defer elective and non-urgent visits to minimize unnecessary exposures while streamlining access to care when needed. Clinics are encouraged to use telemedicine resources when possible to minimize risk of transmission.
-
- CDC Resource for Clinical and Healthcare Facilities: https://www.cdc.gov/coronavirus/2019-ncov/healthcare-facilities/index.html
- NCOPE Statement on O&P Education and Essential Services: https://ncope.org/index.php/2020/03/23/ncope-position-statement-on-orthotic-prosthetic-and-pedorthic-education/
- AOPA COVID-19 Response and Resources: https://www.aopanet.org/resources/covid-19/
- Telemedicine Guidelines & Managing Challenges: Telehealth Guidelines – UW – Mar 2020
- Graciously provided by Dawn Ehde, PhD, Rehabilitation Pyschologist
Legal and Regulatory Considerations
Employees, including most residents are bound by local, state, and federal labor laws. NCOPE cannot regulate hiring or employment related issues, but we ask that residents, residency program directors/mentors, and staff act in alignment with the ABC Code of Professional Responsibility – Section C.4.1: Dignity.
The ABC Credential Holder has the personal responsibility to conduct themselves in a manner that will assure the dignity and status of the Profession.
-
- ABC Code of Professional Responsibility: https://www.abcop.org/WhoWeAre/Documents/Code%20web%20version.pdf
In the event a company can no longer retain a resident due to extenuating circumstances, we kindly ask that the resident(s) affected be given time to make arrangements and any non-compete documents be nullified to allow the resident to pursue any other residency opportunity.
The NCOPE Orthotic/Prosthetic Residency Standards
Residency cannot begin until the prospective resident completes an accredited master’s level O&P education. COVID-19 may affect the graduation dates for currently enrolled practitioner level O&P students. At the earliest, a residency program may begin the day after the date of degree conferral and a residency program may begin on any day of the calendar year.
The minimum length of an orthotic or prosthetic (single-discipline) residency must be 12 months and a combined (dual-discipline) residency must be 18 months for full-time residents. A residency program may be extended with no additional fees to enable the resident(s) adequate time to achieve the requirements defined in the NCOPE Orthotic/Prosthetic Residency Standards. Under no circumstances will the residency be marked complete if the minimum program length is less than 12 months for a single-discipline residency or 18 months for a dual-discipline residency.
-
- We recognize that residents benefit and require time off for rest, illness, and personal needs. Up to 4 weeks (20 business days) of time off can be taken by the resident in addition to any federal holidays observed when the office is closed without the need to extend the residency program.
- Residents have the ability to place their residency on hold for up to 12 months due to extenuating circumstance such as the need to care for a family member, report for active duty military service, or the need to close the clinic where the residency is taking place for an extended period of time.
- For residents who need to extend their residency due to challenges posed by COVID-19, Standard 2.1.3 which defines the maximum residency duration of 24 months for single-discipline and 36 months for dual-discipline residency programs will be lifted allowing programs to be extended further.
A full-time resident is employed a minimum of 37.5 hours per week. In the event the resident’s hours exceed 37.5 hours per week, NCOPE will recognize resident employment beyond 37.5 hours per week to make up for weeks that the resident was employed and their work hours fell below 37.5 hours per week due to the COVID-19 pandemic if extended work hours are allowed by the organization and there is substantial evidence to demonstrate the aditional hours. Recognition of additional hours cannot be leveraged to shorten the minimum residency program duration of 12 months for single-discipline residents or 18 months for dual-discipline residents.
-
- In order to claim hours beyond 37.5 hours per week, the resident must be able to provide all of the following:
- A copy of the residents schedule for each week the resident is claiming more than 37.5 hours.
- Patient names should be redacted, but the date/time/length of the visit, O&P device, and visit type must be clearly visible.
- 100% of cases seen during the weeks where hours exceeded 37.5 hours must be logged within NCOPE Tracker.
- If the resident case load is reduced, non-clinical activities (for example taking an online course) will be need to be logged using the new “Non-Clinical Activity Documentation Form” within NCOPE Tracker.
- The residency director and resident must sign an attestation form verifying that they have reviewed the hours claimed and concur with the documentation provided by the resident.
- The attestation form will be integrated into NCOPE Tracker via the existing “Quarterly Evaluation of the Resident” and “Quarterly Evaluation of the Residency Program” forms.
- A copy of the residents schedule for each week the resident is claiming more than 37.5 hours.
- In order to claim hours beyond 37.5 hours per week, the resident must be able to provide all of the following:
The attestation and fields to upload the redacted schedules is located inside of the Quarterly Evaluation of the Residency form within NCOPE Tracker.
The inability to provide the information listed above will require residents with reduced hours to extend their residency to compensate for the decreased number of hours accrued.
-
- NCOPE cannot define compensation requirements for overtime as they are regulated by local, state, and federal laws. Please consult local legal resources for additional guidance.
NCOPE Resident Decision Tree
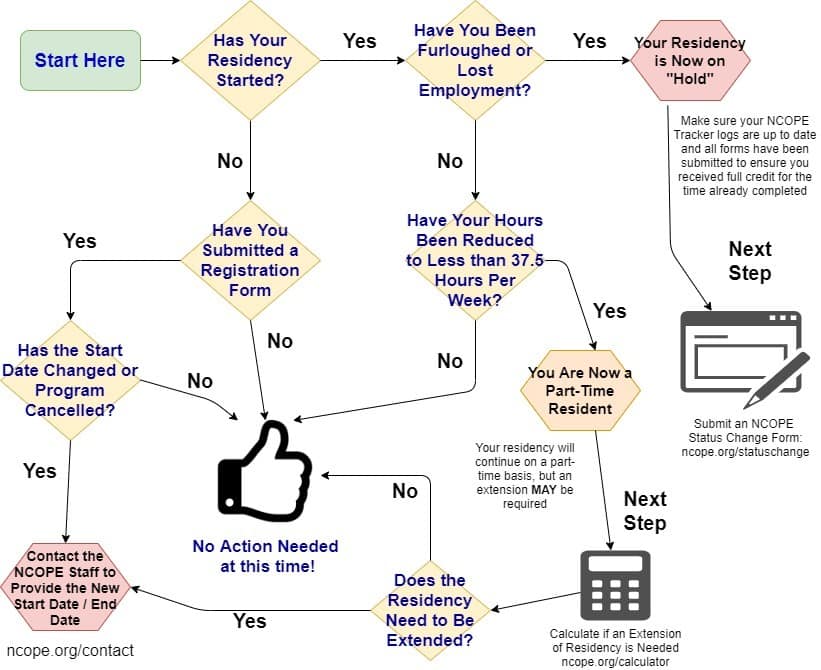
-
- To assist in determining the outcome of a change in average hours per week, furlough, or loss if employment, please visit the Residency Program Duration and Experience Calculator.
- To document a change in residency (for example placing it on hold or heaving a residency end prior to completion), please complete the Residency Status Change Form.
The NCOPE Residency Standards do not define a minimum number of patient encounters at any point during the residency. Residents are required to log every patient encounter greater than or equal to 15 minutes for their currently enrolled discipline(s) using NCOPE Tracker. Any thresholds that report a number of encounters within NCOPE Tracker are intended to simplify the review of report and dashboard tools.
-
- The resident and residency director/mentor must still ensure that all required interventions and patient populations (pediatric/adult/geriatric) are encountered and documented using NCOPE Tracker in order for a residency to be deemed complete.
NCOPE Residency Requirements and Competencies
The resident must attain required orthotic and/or prosthetic competencies in order to have their residency deemed complete. A shortfall of real-world patient encounters may exist for elective/non-urgent care at this time, but these patients will eventually return to the O&P practices. It may be necessary to have the resident rotate through a different facility via an affiliation agreement should local regulations or limitations in patient populations prevent the resident from seeing a specific intervention at the primary residency site.
It is important to recognize that not all of the knowledge and skills required to achieve competency must be developed in the physical presence of a patient. The skills of assessment, development of treatment plan, casting/measurement, fabrication, and practice management can be practiced on a healthy person or discussed as a case study between the resident and their director/mentor.
- Practicing the above skills outside of a real-world patient care setting is not intended to replace direct patient encounters but help prepare the resident to be engaged at a higher level when future opportunities do present. This approach also creates an environment potentially less stressful than developing these skills for the first time on an actual patient.
- Retrospective chart reviews enable the resident to review an entire episode of care in a single sitting, plus the documentation can be assessed against supplier standards for compliance.
The Quarterly Evaluation of the Resident and Quarterly Evaluation of the Residency Site/Mentor are relevant and must be completed even if there are limited patient encounters. These forms do not focus on a specific device types, diagnosis, or age groups but instead the opportunities for learning which occur inside and outside of the patient care area.
Quarterly Clinical Track Activities and Quarterly Research Updates must be submitted to deem the residency complete. For residents affected by the COVID-19 pandemic, NCOPE will allow residents to complete multiple quarterly clinical track projects or engage is a focused period of research when access to patient care opportunities is limited. Early submission of quarterly clinical track activities or research components will enable the resident to focus on patient care once the patient volume begins to increase.
Residents can gain valuable knowledge from continuing education courses. Both the Academy (AAOP) and The American Orthotic Prosthetic Association (AOPA) may offer continuing education opportunities including many that are free if no CE units are being pursued. Downtime in the clinic may create the opportunity for the resident to develop knowledge on patient populations or interventions that are not plentiful when patient volumes are normal.
-
- AAOP Online Learning Center: http://oandp.org/olc
- AOPAversity: https://www.aopanetonline.org/aopaversity
Resources
- The NCOPE O&P Education Resource Database – Accounts are available for both residents and mentors/directors
- To create a new account or login to an existing account, please visit: https://ncope.org/index.php/login-page/
- The Academy is offering from access to OLC courses through May 31, 2020 for all students and residents.
- For non-members, they can request an account by clicking HERE.
- For additional information, please email: info@oandp.org
- The Center for Creative Leadership – Leadership Resources for Times of Crisis: https://www.ccl.org/coronavirus-resources/
Revision Notes
4/2/20 – Additional resource section amended and links for the online residency status change form were amended.
4/7/20 – The residency program duration / experience calculator and status change form links were appended.
4/13/20 – The residency status flow chart graphic was appended.
4/17/20 – The Education Events List was appended to resources.
4/28/20 – Clarifying information was added to discuss the documentation of non-clinical activities in addition to residents requesting acknowledgement of hours beyond 37.5 hours per week.
5/15/20 – Details were provided about where residents will upload de-identified schedules and attest when requesting hours beyond 37.5 hours per week be recognized.